RWJF’s Approach
This framework offers insights into what elements drive successful efforts to align the health care, public health, and social services sectors. A printable version of this framework is available in the Resource Library.
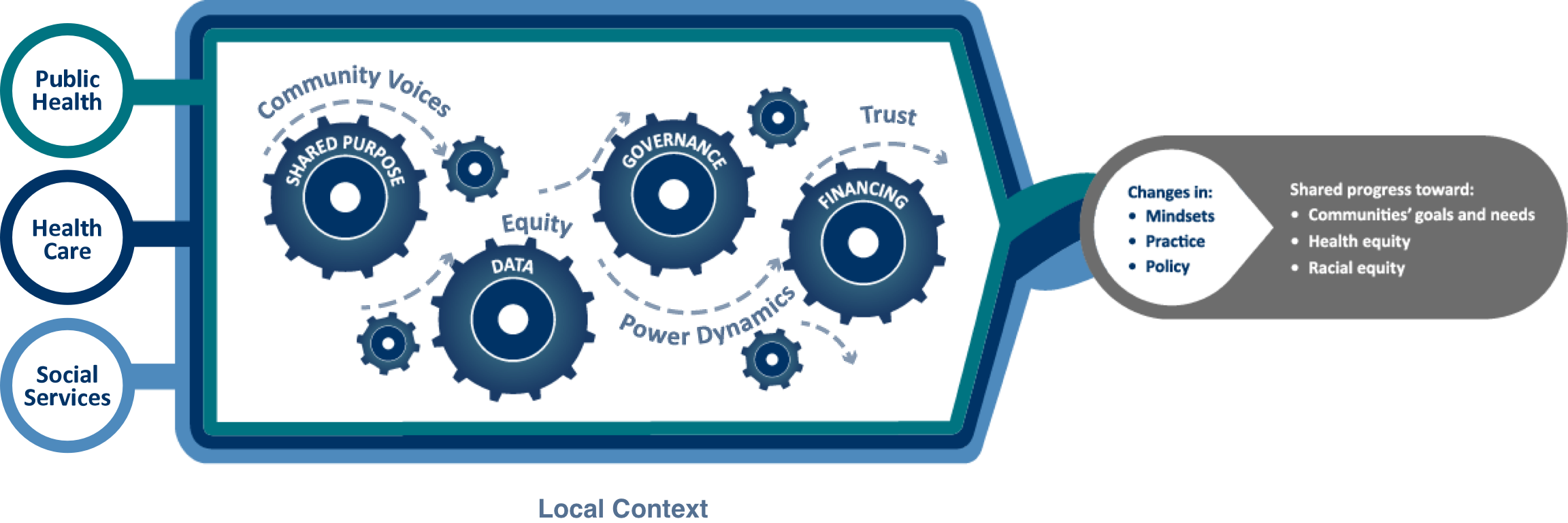
This framework offers insights into what elements drive successful efforts to align the health care, public health, and social services sectors. A printable version of this framework is available in the Resource Library.

“Strategically designing and connecting a community’s health improvement efforts across all major institutional players … offers great promise.”
-ReThink Health
Bringing together sectors requires navigating power dynamics, trust imbalances, and other factors. As ReThink Health notes, even the most mature multisector partnerships can face an uphill battle to advance their ambitions. Over the last decade, RWJF and other organizations funded many individual initiatives and projects to align sectors. These efforts identified practical learnings such as “what works” and “pitfalls” in designing aligning efforts (via the Center for Community Development Investments) and the important roles of upfront relationship-building, common vision, active champions, and formal partnerships (via the Partnership for Healthy Outcomes).
The COVID-19 pandemic has brought a sense of urgency that has fostered cross-sector innovation around key problems, including addressing food insecurity in Sacramento, California (via Public Health National Center for Innovations), improving mental well-being and housing in Hennepin County, Minnesota (also from Public Health National Center for Innovations), and leveraging care coordination services in Pierce County, Washington (via Aligning Systems for Health).
A town in Westchester County, New York, was the epicenter of the state’s earliest COVID-19 outbreak. The National Center for Complex Health and Social Needs describes how a new cross-sector coalition convened to address food insecurity caused by a rise in unemployment. Volunteers purchased meals from local restaurants and delivered them to families facing hunger. As the case study notes, “even as restrictions lift and individuals return to work, the coalition, informed by the unprecedented experiences that COVID-19 has brought, will continue its work and use its momentum to identify shared solutions to some of the most challenging issues in [the] community.”
“Measurement can reinforce the status quo or be a force for change.”
-American Institutes for Research
The health of an individual or community is affected by myriad factors—from housing and access to food to education and transportation—yet data systems are historically contained within a sector or even a single organization with little sharing. Successfully addressing complex challenges that affect community health such as maternal and infant mortality or the opioid epidemic requires having shared data and measurement systems to gather, organize, and share data between entities. This can effectively coordinate activities and use information to track shared progress towards equitable outcomes.
There is no one-size-fits-all approach for such a system, which can range from a hospital and social services organization incorporating social determinants of health data into an existing electronic health record to a community coming together to create an entirely new dashboard.
Aligning Systems for Health notes that data is inextricably linked to other elements of the framework. Data is a driver of collaboration steering nearly all aspects of aligning systems, particularly purpose and governance. Effective use of data, for instance, can ensure an equitable response to long-standing challenges.
In communities nationwide, information-sharing across sectors is informing an equitable COVID-19 recovery (via American Institutes for Research), addressing food insecurity in Texas (via Aligning Systems for Health), improving literacy (via American Institutes for Research), decreasing rates of infant mortality in Ohio (via Aligning Systems for Health), and much more.
Data Across Sectors for Health shares an example from Los Angeles County of a person experiencing homelessness who misses a health care appointment. Perhaps this absence isn’t noteworthy or could be attributed to lack of transportation or last-minute conflict. A shared data system, however, shows that this person spent the previous night in jail. Stepping back further, data reveal the client missed 10 prior mental health appointments. With a shared data system, the care team can determine the underlying complications faster and develop better solutions—all thanks to data sharing.
“The actual structure still exists. The idea still exists. The question is, ‘How do we go on from here without continued funding?’”
-Healthy Homes Des Moines
Aligning sectors strives to create partnerships that are “built to last.” Yet it is challenging to aim for sustainability or even keep the lights on when funding sources are unknown. While experts convened by Aligning Systems for Health caution there is a lack of collective knowledge and meaningful conversation about sustainable financing structures (which may be because such efforts are in early phases), many communities are effectively navigating this journey.
Sustainable financing includes appropriate incentives and shared accountability. It can be approached from three perspectives: sources, uses, and structures. Often there is a combination of public-sector funds like Medicaid waivers, philanthropic support (including grants), and community-based financing mechanisms like community wellness funds that can help bring in money to get aligning efforts off the ground.
In communities nationwide, sustainable financing is transforming health though building a vibrant Michigan economy (via Aligning Systems for Health), addressing Coloradans’ social needs in health plan payments (via Aligning Systems for Health), creating permanent housing post-Hurricane Katrina (via Center for Health Care Strategies and Better Health Beyond Health Care), addressing new strategies to care for individuals with complex health and social needs (via Advancing Integrated Models), and much more.
For years the Oregon Health Authority and federal Medicaid funds have entirely financed the Yamhill Community Care Organization (YCCO) as a result of meeting care metrics outlined by the state. Aligning Systems for Health describes how YCCO’s board of directors makes the final payout determinations, but YCCO typically reinvests the funds back into the community through programs run by contracted partners that address social determinants of health, including housing, food insecurity, and education.
“Governance functions ensure accountability, transparency, and fairness across the various groups that are collaboratively stewarding transformative work in their region.”
-ReThink Health
Good governance to guide efforts is necessary for successful cross-sector alignment, per research by the Center for Sharing Public Health Services and Public Health National Center for Innovations. This includes establishing and maintaining clear and appropriate roles, defined leadership and relationships, decision-making processes, data-sharing arrangements, and collaboration authority.
When aligning sectors, a backbone organization is often identified or newly formed to serve a leading role, such as the Atlanta Regional Collaborative for Health Improvement. Such an entity, as Aligning Systems for Health explains, can leverage existing infrastructure and resources while remaining impartial, propelling efforts forward effectively.
Early governance activities often include developing partnership agreements or memorandums of understanding, determining the role and appropriate representation of an advisory group or board, and agreeing on policies and procedures.
Strong governance is improving access to healthy food in Albuquerque (via BUILD Health Challenge), meeting the health and social services needs of LGBTQ youth in Detroit (via Center for Health Care Strategies, Nonprofit Finance Fund, and Alliance for Strong Families and Communities), developing approaches for whole-person coordinated care in Trenton, New Jersey (via Data Across Sectors for Health), and much more.
Aligning Systems for Health highlights how in King County, Washington, HealthierHere works across sectors to build an accessible and integrated services delivery system, with the ultimate goals of reducing health disparities, improving health outcomes and client experiences, and reducing per-capita costs. A leader of the organization credits its neutrality as a “secret ingredient” to its ability to work across sectors.
HealthierHere is governed by a 26-member cross-sector board in which the members represent their sector rather than organization, which encourages broad engagement and results in widely attended open board meetings. Board seats are divided equally among community members, social services agencies, and tribal partners; hospital systems, community health centers, and community behavioral health agencies; and government, payers, and philanthropy.
“Aligned systems use a shared purpose to reach across the boundaries of their existing organizations to do something bigger together.”
-Aligning Systems for Health
Efforts to align sectors are often initiated by external factors, according to Aligning Systems for Health, including overcoming a significant challenge (e.g., cost, efficiency, inequity), a philosophical or historical value (e.g., service to a vulnerable population), or an external or internal nudge (e.g., pandemic response, legislation, vision of a new leader, or sustainability concerns).
Yet without a mutual understanding and commitment to a vision and priority outcomes, aligning efforts will only get so far. As JSI finds, purpose is foundational to aligning sectors and requires significant time and resources. Once this is determined, meaningful work can begin.
Shared purpose across sectors is addressing the struggles of the “working poor” in Idaho (via Aligning Systems for Health), assisting community workers in Philadelphia handling nonmedical issues during the COVID-19 pandemic (highlighted by Health Affairs), showing how children’s hospitals can spur alignment (via Health Leads), improving the health and well-being of Medicaid beneficiaries (via Center for Health Care Strategies), and much more.
Like in so many communities, organizations in Lake County, Colorado, previously conducted independent needs assessments and addressed the findings in siloed, disparate ways. Understanding the opportunity to combine forces, sector leaders convened and launched the Health and Happiness Project, which shapes community-wide priorities and guides how health care, public health, and social services can align efforts to achieve the greatest health for the most community members. At the heart of the planning process are the residents who voice their opinions in short online surveys and community meetings to determine which social, environmental, and economic factors to prioritize. Through this process, Lake County is tackling upstream determinants of health including affordable housing, a living wage, and child care.
“Given variance in the local context, there is no single model or formula to align systems. However, there are commonalities that drive successful efforts.”
-Aligning Systems for Health
Each community is unique in its specific strengths and challenges. What works for one community to align sectors may not work for another, given the dynamic nature of communities. These local factors play a critical role in if and how aligning is embraced by sectors, organizations, leaders, and community members.
Experts convened by Aligning Systems for Health note that external drivers often accelerate alignment activity, such as a health-related crisis (like the COVID-19 pandemic or opioid epidemic) or state or federal policy opportunities for aligning (such as the Accountable Health Community model or American Rescue Plan Act funding).
Likewise, internal capacity can enhance or inhibit aligning efforts. Having committed leadership, a workforce with appropriate skills, and strong backbone capabilities can set communities on a positive path forward. On the other end, constant turnover, lack of training, and conflicting priorities can hinder such work.
In tandem with local factors, internal and external drivers are empowering sectors to support people without homes during the COVID-19 pandemic in Atlanta (via Aligning Systems for Health), address opioid abuse and prevent overdose deaths in Ohio with support from the governor’s cabinet (via Center for Health Care Strategies and Better Health Beyond Health Care), and more.
For many states the COVID-19 pandemic is driving new and existing collaboration between sectors and systems. Aligning Systems for Health describes how CARES Act funding enabled North Carolina to launch a community health worker initiative after years of planning. As part of this effort, more than 400 community health workers are being hired to immediately assist with COVID-19 contract tracing. In the long term these community health workers connect individuals with resources for health care, food, housing, employment, and other health and nonmedical needs.
“We’ve had to abide by the values that we set up with those residents when we started. And their voice is the one that should take precedence.”
-BUILD Health Challenge
When the community has a say, substantive change can happen. Elevating these voices ensures lasting improvements are driven by and for the community. This is particularly true for improving health locally as the health care, public health, and social services sectors are working together in new ways.
Active community engagement ensures its members are heard and integrated in the design process at the beginning of an effort and remain involved throughout. Taking these steps builds trust and addresses long-standing power dynamics that have silenced these voices in the past.
Experts note that having representatives from community-based organizations is not the same as having community members at the table, and community engagement is not synonymous with community leadership.
By elevating community voices, aligning efforts are leveraging county and tribal health councils to advance a Culture of Health in New Mexico (via Community Voices for Health), reducing obesity rates in Gastonia, North Carolina (via BUILD Health Challenge), and supporting youth in distressed Mississippi communities to succeed in school and beyond (via Aligning Systems for Health).
From its conception the Healthier Together initiative in Palm Beach County, Florida has empowered residents to be at the center of systems change, neighborhood by neighborhood. Aligning Systems for Health details how the resident-led approach intentionally incorporates community voices in setting priorities, sense-making around data, guiding grant funding decisions, and serving on the project steering committee, which is comprised of an equal proportion of lived leaders and learned experts.
“Equity can be a process or an outcome, but in either case, it is widely understood to be critical for cross-sector aligning and, ultimately, for improving community well-being.”
-Aligning Systems for Health
Addressing equity in the context of both health and race is a critical goal of aligning across sectors and, ultimately, critical for improving community well-being.
Health equity tailors support for each community so everyone who lives there has the same opportunity to live the healthiest possible life. Unlike equality, which provides everyone with the same resources, equity acknowledges that distinct communities and individuals face unique barriers and require assistance to achieve equal footing.
Centuries of racism and discrimination—including systemic, institutional, and individual barriers that deny equal opportunity to groups based on race or ethnicity—result in worse health outcomes, including shorter life expectancy for Black and brown individuals in the United States. Equity-driven initiatives work to correct systemic barriers and level the playing field.
Aligning Systems for Health highlights common barriers and strategies to improve equity, reduce structural racism, and ultimately diminish or eliminate persistent health disparities. Strategies at the individual, organizational, and systems level range from empowering social workers at the decision-making level to implementing Health in All Policies.
While equity is viewed as a “cross-cutting” principle influencing aligning, researchers funded by Aligning Systems for Health find that two primary issues arise when considering equity: a lack of clarity about its definition and uncertainty about operationalization.
By prioritizing equity, aligning efforts are guiding the nation’s COVID-19 response and recovery (via Aligning in Crisis), managing housing during COVID-19 and beyond (via Data Across Sectors for Health), and improving active transportation options in California (via Center for Health Care Strategies and Better Health Beyond Health Care).
Guided by Aligning Systems for Health, national experts outline how local context and interrelated factors play a role in aligned systems advancing health equity and addressing systemic racism:
“People with the least power are often closest to the problems.”
-Aligning Systems for Health
Aligning across sectors can be challenging because of inherent power imbalances between the sectors and between organizations and individuals. These differences in power can result from imbalances in resources, perceived value, historical practices, influence, or experience.
Research shows that the people with the least power are often most affected by the problem. This is particularly important because people are more likely to adopt change when they are involved in the process.
Power dynamics are at play in every interaction when aligning sectors, in ways visible (e.g., who is and is not represented on an advisory committee) and invisible (e.g., which sector brings the most money to the table). Successful efforts to align sectors must acknowledge power dynamics and work to level the field.
Intentionally shifting power dynamics is empowering neighborhood-by-neighborhood health improvement efforts in Florida (via Aligning Systems for Health), helping children thrive in Cincinnati (via Health Leads), and addressing food insecurity through economic partnerships in California (via Public Health National Center for Innovations).
Minutes west of Charlotte, historical disinvestment in Gastonia, North Carolina resulted in mistrust and challenging conditions. To address upstream factors of health disparities like racism and inequitable food access, Healthier Highland convened sectors and partners to work together in new ways. The effort intentionally shifted power to the community by engaging resident-leaders, building a neighborhood association, strengthening local partnerships, and hiring a well-respected community member who understood the power dynamics in the community and broader context to lead the cross-sector effort.
“Building trust means moving collectively from the Comfort Zone to the Learning Zone.”
-Aligning Systems for Health
Trust, both with the community and between organizational partners,plays a foundational role in aligning sectors and must be built intentionally. Trust is critical to maintain connections, build community, and leverage success.
Two types of trust, relational and transactional, are necessary in collaborative efforts. Relational trust is earned through shared experiences and backgrounds, while transactional trust is earned through positive interactions. Trust may need to be rebuilt or regularly renewed.
Without trust other elements of aligning sectors are not possible. Research funded by Aligning Systems for Health is studying the role of trust and best practices for building and restoring it. JSI, for instance, notes the primary outcome of the collaborative formation stage should be increased trust, and this will grow and inform all other aspects of aligning.
Relationships based on trust have made strides in leveraging data to address social determinants of health (via National Center for Complex Health and Social Needs), fostering hospital-community partnerships (via American Hospital Association and Health Research & Educational Trust), and advancing community transformation and economic development (via Aligning Systems for Health).
Partners and community members alike may be cautious when sharing data, but foundational trust can ensure data are used in an effective and ethical way. Using real-world learnings from AllianceChicago, the Camden Coalition of Healthcare Providers (New Jersey), and the Providence Health and Services Center for Outcomes Research and Evaluation (Oregon), the National Centers for Complex Health and Social Needs highlights six strategies to achieve this, ranging from building on existing partnerships to understanding that building collaborative relationships takes time.
“The process of aligning across sectors may create pathways for different conversations, new perspectives, better listening, and a way to challenge the status quo.”
-Aligning Systems for Health
When sectors work together in ways that are built to last, true change is possible. Achieving strong, lasting connections across systems helps build healthier and more equitable communities.
The sectors already have the expertise needed between them. Aligning sectors will improve how they work together to better support the people they serve and tackle complex, community-level barriers to good health, especially for people who find it hard to stay healthy, safe, and make ends meet.
To do so requires fundamentally reshaping policies, programs, and practices. Ultimately this will lead to a new paradigm that promotes health equity and reduces systemic racism, allowing every person in the United States to have a fair and just opportunity for health and well-being.
Experts convened by Aligning Systems for Health categorize aligning outcomes in three ways:
Much like for Destiny and other new mothers in Arkansas, the Home Together program has been a lifeline for those in vulnerable communities, including underrepresented racial minority groups. A case study developed by Aligning Systems for Health shows how the program aligns the health care, public health, and social services systems to ensure that newborns leave the hospital for a safe, healthy, and stable home environment. Without it families may bounce between relatives’ houses or live on the street.
While there have been many process and project successes along the way, perhaps the most meaningful has been the effect on families. The first 78 mothers to receive six-month follow-up assessments showed an improvement in nearly every indicator measured, including housing status, mental health symptoms, and access to health care. As Destiny says, “This is just the beginning for me.”